Tan Sri Dr. Noor Hisham, Malaysia’s Director-General of Health, estimates that 3.9 million individuals, or 20% of Malaysia’s adult population, are diabetes patients. According to the National Health and Morbidity Survey Report, the percentage of adult Malaysians with diabetes has significantly increased, going from 11.2% in 2011 to 13.4% in 2015 and 18.3% in 2019. Nevertheless, more than 30% of Malaysians are unaware they have been diagnosed with diabetes. The gender split of the 1.7 million diabetes patients in 2020 was 57.02% female and 42.98% male.
The majority of individuals don’t realize they have diabetes until they start experiencing common symptoms, which include eating more, drinking more, urinating more, or losing weight. This is because there aren’t any evident signs of diabetes in the early stages. They cannot control blood sugar in time, as they are not discovered in time and lead to comorbidities. Early treatment is required in cases with metabolic abnormalities and the three-hypers – high blood pressure, high cholesterol, and high blood sugar – in order to prevent diabetes and other cardiovascular diseases.
Younger Diabetics
Diabetes has evolved from a common disease to a severe societal issue with numerous comorbidities and complicated variables as Malaysia enters an aging society. In Malaysia, the rise of young diabetics is another significant issue. More than 7 million people are predicted to have diabetes by 2025, with a 31.5% prevalence among Malaysian adults across the country.
Young-onset diabetes (YOD) refers to type 2 diabetics who age below 40. Many countries have found that YOD prevalence has been rising drastically in recent years; however, the factors are yet to be confirmed. Studies have shown that Africans and Asians have a higher YOD prevalence than other ethnic groups.
Diet Control and Exercise
Other than medical treatment, diet control and exercising frequently are also crucial to recovering from type 2 diabetes. Younger type 2 diabetic patients are more likely to be out of control than the elderly, due to the rapid aging of insulin cells and more consequential complications.
Continuous Monitoring of Blood Sugar Levels
Weight management is the key to preventing diabetes and three-hypers. Nowadays, the number of overweight and obese individuals is rising. Thus, it is significant for us to lose weight in order to achieve a healthy lifestyle and reduce the demand for medication intake.
In addition, monitoring blood sugar levels continuously can help us improve diabetes. In the past, insulin intake was the only way to cure diabetes. However, research in recent years has shown that drugs, injections, oral incretins, or even continuous blood sugar level monitoring can help us improve type 2 diabetes.
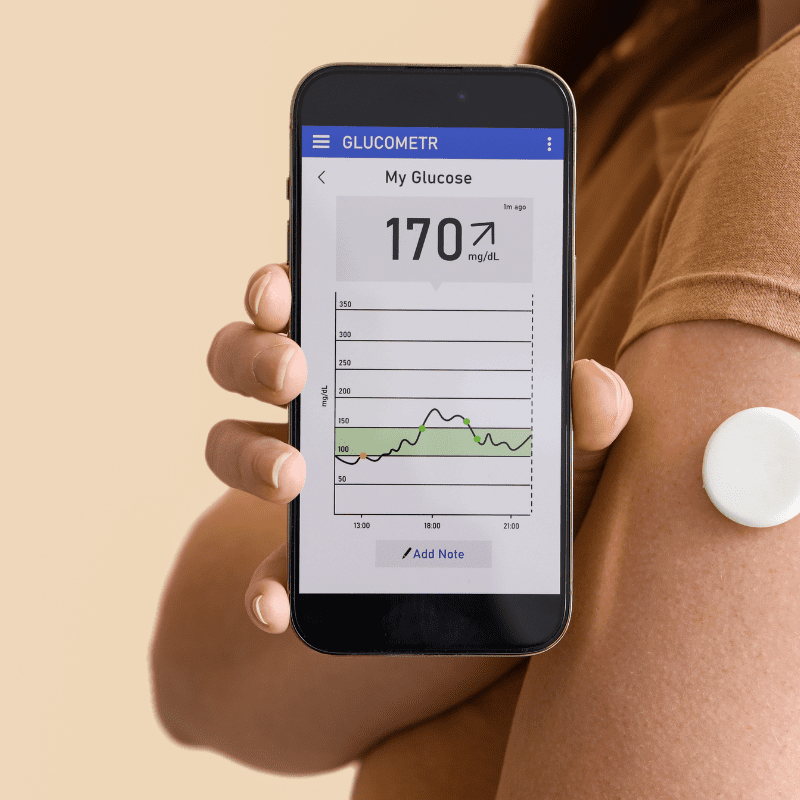
What is A Blood Sugar Detector?
Medical staff will install an automated blood sugar detector under the skin by using a thin blood sugar-sensing needle. It can automatically monitor the blood sugar level in the subcutaneous tissue fluid and record it on the receiver via Bluetooth. By recording data such as diet content, exercise pace, and medical records, patients are able to notice the concentration of blood sugar at any time. A home blood sugar test apparatus has similar properties to an automatic blood sugar level detector, too. In actuality, blood sugar levels can only be monitored manually, in contrast to an automated blood sugar meter. Patients cannot detect changes in blood sugar without spilling a drop of blood on the monitoring device.
In addition, every diabetic patient has to have their medication dosage precisely adjusted by a specialist. Therefore, an autonomous blood sugar level meter can help clinicians by properly tracking patient blood sugar variations. Patients can also alter or enhance their lifestyle by being aware of blood sugar variations.
5 Types of Diabetic Patients
- New patients with frequent and recurring hypoglycemia.
- Blood sugar fluctuates greatly, especially at midnight.
- Those with diet control but not an ideal glycosylated hemoglobin level.
- Changes in exercise intensity, illness, or infection.
- Glycosylated hemoglobin levels increased unexpectedly.
Diabetic patients who lack blood sugar control may experience various complications. For instance, cerebrovascular disease, cardiovascular disease, retinopathy, peripheral vascular disease, neuropathy, and a weakened immune system.
Relationship between Hepatitis C and Diabetes
Diabetes is the main Hepatitis C comorbidities. Studies have shown that the prevalence of hepatitis C in diabetic patients is about 2-3 times that of the general population. The risk of hepatitis C infection leading to diabetes has even increased by 11 times.
Hepatitis C causes chronic inflammation throughout the body and blood vessels, although it mainly infects liver cells. Studies have found that the hepatitis C virus can cause insulin resistance, increase blood sugar, blood pressure, and blood lipids, and also cause damage to endothelial cells, eventually leading to cardiovascular disease, stroke, and other diseases.

